|
| This post was peer reviewed. Click to learn more. |
Author: Eric Sulava, MD
Emergency Medicine Resident
Naval Medical Center Portsmouth
AAEM Education Committee
Author: Hannah Harris MD
Student Naval Flight Surgeon
Naval Aerospace Medical Institute
Author: Katrina Destree, MD
Staff Physician
Naval Medical Center Camp Lejeune
Chief Complaint
“My heart was racing and then everything went grey”
History of Present Illness
A 21 year old otherwise healthy male, presents to the Emergency Department (ED) following an episode of syncope with forehead laceration. He reports brushing his teeth, when he suddenly had a “wave of anxiety” rush over him. He noticed a few seconds of palpitations and then remembers washing his bloody hands in the sink. When looking at the time, he had lost 4 hours of time. He denies personal or family history of seizure disorders; and did not experience incontinence, tongue biting, or a post ictal period. He currently denies chest pain, pleuritic pain, shortness of breath, constitutional symptoms, lightheadedness, neck pain, headache or any other neurologic sequelae.
Physical Exam
VITALS: BP: 110/63, Pulse: 104, Temp: 98.6, RR: 20, SpO2: 98% on room air
GENERAL: No distress, well appearing male
NEURO: Alert and oriented, normal strength (5/5) all extremities, normal sensation, cranial nerves intact, finger to nose without dysmetria, no pronator drift
HEENT: Left facial tenderness over a small, linear 2 centimeter forehead laceration. No other abnormalities
RESPIRATORY: Breath sounds clear and equal bilaterally
CV: Tachycardic, regular rhythm, no murmurs, rubs or gallops
ABDOMEN: Soft non-tender, non-distended
SKIN: Warm and dry with no evident rash
Case Discussion
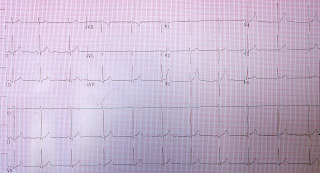
Given the patient’s concerning history of sudden loss of consciousness, a cardiogenic and neurologic syncope workup was initiated. The patient’s complete blood count, complete metabolic panel, thyroid stimulating hormone, troponin, d-dimer, urinalysis, urine drug screen, and computed tomography of the head were unremarkable. The sole abnormality of the initial evaluation, was a sinus tachycardia with a shortened PR interval, and normal QRS.
The history of periodic palpitations with syncope led to concern for a recurrent pre-excitation syndrome with decompensation to a non-perfusing rhythm. Cardiology was consulted and further diagnostics were ordered. A holter monitor was placed, which is pending. The patient’s echocardiogram was unremarkable. Neurology completed a brain magnetic resonance image (MRI) and Electroencephalography (EEG), without attributable findings. He is currently pending further EP studies.
The term “pre-excitation syndrome” defines all conditions in which ventricular or atrial activation occurs through an anomalous pathway. Although most commonly describing Wolff-Parkinson-White (WPW), this term also covers Lown–Ganong–Levine (LGL). WPW is characterized by a short PR interval and a wide QRS complex. This QRS lengthening is due to the “delta wave”, representing atrioventricular node (AV) bypassing through an accessory pathway called the Bundle of Kent [1]. LGL is a clinical syndrome consisting of intermittent tachycardia with the electrocardiogram (EKG) findings of a short PR interval and normal QRS complex. The shortened PR is secondary to a lack of AV nodal blockade, theoretically explained by intranodal or paranodal fibers that bypass all or part of the AV node [2,3].
Lown, Ganong, and Levine conducted a retrospective analysis of 13,500 consecutive EKGs, finding 200 subjects with a shortened PR interval. This study, completed in 1952, showed that the incidence of paroxysmal supraventricular tachycardia (SVT) was significantly higher in patients with a shortened PR interval [2]. This clinical description was formed before the development of EP studies, therefore subsequent studies have attempted to attribute a structural anomaly to the clinical syndrome. James fibers (trans- AV nodal fibers), Mahaim fibers (muscular bridges), Brechenmacher-type fibers (atrium to the His bundle connection) have been identified histologically, but have not been uniquely connected to the tachyarrhythmia syndrome of LGL [4,5]. Due to the difficulty with identifying a unique pathophysiologic root for the LGL syndrome, there is little data to further validate association between LGL and sudden cardiac death or SVT.
The primary goal of ED evaluation will be stabilization, risk stratification, and monitoring. As mentioned above, a wide differential is warranted in any syncope patient, and all life threats should be initially excluded. Further management of isolated LGL will involve the aid of a cardiologist, to determine the need for non-invasive mapping of the arrhythmia. Like WPW, ED providers should take caution with sympathomimetic agents, which could increase the risk of tachyarrhythmia. Unfortunately AV nodal blocking agents and antiarrhythmic drugs have not been extensively studied in LGL. The effects of beta blockers and calcium channel blockers have varied widely with no official recommendations (6,7). Recently, catheter ablation has become the preferred therapy for various SVT, showing the utility of early involvement from the cardiologist [8].
Pearls
- Pre-excitation syndrome describes both WPW and LGL
- WPW is characterized by a short PR interval and a wide QRS complex
- The “delta wave” represents atrioventricular node (AV) bypassing through the accessory Bundle of Kent
- Historically, SVT is significantly higher in patients with a shortened PR interval
- Keep a wide differential on syncope patients, to include subtle EKG findings
Questions
- What abnormalities are seen in the above electrocardiogram (EKG)?
- What are the not-to-be-missed arrhythmias in young adults with syncope?
Answers to above Questions
- Shortened PR interval and normal QRS: suggestive of Lown-Ganong-Levine syndrome (LGL).
- Long/short QT syndrome, Brugada syndrome, Pre-excitation syndrome (WPW, LGL), arrhythmogenic right ventricular dysplasia, Paroxysmal supraventricular tachycardia (SVT), and ventricular tachycardia.
Resources:
1. Stapczynski J, Cline D, Ma OJ et al. Chapter 18: Cardiac Rhythm Disturbances. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8th edition. McGraw-Hill Education / Medical; 2015.
2. Lown B, Ganong WF, Levine SA. The syndrome of short P-R interval, normal QRS complex and paroxysmal rapid heart action. Circulation. 1952;5(5):693-706.
3. Benditt D, et al. Characteristics of Atrioventricular Conduction and the Spectrum of Arrhythmias in Lown-Ganong-Levine Syndrome. Circulation. 1978: 57( 3):454–465.
4. Mandel W J, et al. Lown-Ganong-Levine Syndrome: A Study Using His Bundle Electrograms. Circulation. 1971: 44(4): 696–708.
5. Durrer D, et al. Pre-Excitation Revisited. The American Journal of Cardiology. 1970:25(6). 690–697.
6. Benditt, D, et al. Chapter 12: AV Node Bypass Tracts and Enhanced AV Conduction – Relation to Ventricular Preexcitation. Cardiac Preexcitation Syndromes. Springer- Martinus Nijhoff Publishing:1986.
7. Seipel L, et al. Atrioventricular (AV) and Ventriculoatrial (VA) Conduction Pattern in Patients with Short P-R Interval and Normal QRS Complex. Cardiac Pacing. Springer, Berlin, Heidelberg:1976.
8. Yeung-lai-wah JA, Alison JF, Lonergan L, Mohama R, Leather R, Kerr CR. High success rate of atrioventricular node ablation with radiofrequency energy. J Am Coll Cardiol. 1991;18(7):1753-8.
I am a military service member. This work was prepared as part of my official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines a United States Government work as a work prepared by a military service member or employee of the United States Government as part of that person’s official duties.
The views expressed in this article are those of the author(s) and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.