 |
| This post was peer reviewed. Click to learn more. |
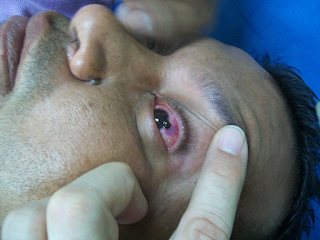 |
| Image credit: Wikimedia Commons |
Author: Conner Murphy, MSIV
Medical Student
Uniformed Services University School of Medicine
Additional Authors:
Ivan Yue, MSIV
Medical Student
Uniformed Services University School of Medicine
AAEM/RSA Publications and Social Media Committee
Melisa Walsh, MSIII
Medical Student
Uniformed Services University School of Medicine
David Supinski, DSc EMPA-C
Emergency Medicine PA
Fort Belvoir Community Hospital Emergency Department
Grigory Charny, MD MS FAAEM
Assistant Professor
Department of Military and Emergency Medicine, Uniformed Services University School of Medicine
Introduction
An open globe laceration is defined as a full-thickness penetration of the eye by a sharp object.[1] Observational studies suggest that male patients ages 10-19 are at highest risk for this type of injury due to types of sports they participate in, occupations, and involvement in physical altercations.[2,3] Obvious signs of trauma are not always apparent, and a negative Seidel’s test does not rule out an occult intraocular foreign body as the wound may temporarily seal itself if small enough.[4] Decreased visual acuity, chemosis, hypotony, and pain are often the only clues that the patient has an open globe injury.[5] Early diagnosis and evaluation by an ophthalmologist are crucial to preserving vision.[6] In this case report we present an atypical case of a 24-year-old male patient with penetrating eye trauma to his right eye that was not apparent on physical exam or computed tomography.
Case Presentation
A 24-year-old male patient presented for right eye trauma from suspected glass fragments following the explosion of a car headlight. Initial exam in the emergency department revealed multiple abrasions around the right eye and diminished visual acuity (right eye: 20/60, left eye: 20/25). Pupillary exam showed no evidence of an eccentric iris or intraocular structure prolapse. Seidel’s test was negative. Computed tomography (CT) imaging of the orbit demonstrated no foreign bodies or open globe injury. Given high clinical suspicion for an open globe injury, pneumotonometry was performed which demonstrated a right-sided intraocular pressure of four mmHg and left-sided intraocular pressure of twenty mmHg. At this point, ophthalmology was consulted. On surgical examination the patient was diagnosed with a full thickness laceration with anterior chamber collapse. The patient subsequently underwent successful surgical repair.
Discussion
Blast injuries are a high-risk mechanism for open globe injuries; in this case glass from an exploding car headlight. Other than decreased visual acuity, there were no physical exam findings suggestive of an open globe. Additionally, CT scan of the eye showed no evidence of an open globe injury. CT scans are 51% to 77% sensitive in the diagnosis of open globe injuries, depending on the reader.[5] As such, CT scan is not recommended as the sole means to rule out an open globe injury. Surgical exploration is the gold standard for evaluation and is recommended for any patient with a high clinical index of suspicion.[5] A decreased intraocular pressure reading via pneumotonometry and decreased visual acuity were the only signs in this case indicating a possible open globe. Tonometry and any other exams or tests that may raise intraocular pressure are usually contraindicated in suspected open globe injuries due to risk of further expulsion of intraocular contents.[7] Pneumotonometry differs from traditional tonometry in that it utilizes a brief puff of air to estimate the intraocular pressure. It is a non-contact device as opposed to traditional Goldmann applanation tonometry or the Tono-Pen device which require direct contact on the cornea. Given this difference in mechanism for obtaining a reading, pneumotonometry was considered to bear lower risk for exacerbating the condition while providing valuable clinical data. However, reports of this technique in occult ruptures are limited; thus, there is a lack of information as to the safety of this approach in patients with an open globe injury.
Conclusion
With high clinical suspicion for globe penetration, a negative Seidel’s test and CT scan cannot be used to rule out an open globe laceration. Pneumotonometry may be considered as a potential tool to determine the intraocular pressure as opposed to direct tonometry to avoid further expulsion of intraocular contents. However, more evidence is needed to determine the safety of this approach in patients with open globe lacerations. Early detection of this injury can lead to prompt ophthalmology consultation, potentially minimizing the long-term complications of an occult open globe injury in an otherwise healthy patient.
Bibliography
- Kuhn F, Morris R, Witherspoon CD, Heimann K, Jeffers JB, Treister G. A standardized classification of ocular trauma. Graefes Arch Clin Exp Ophthalmol. 1996 Jun;234(6):399-403. PubMed PMID: 8738707.
- Blomdahl S, Norell S. Perforating eye injury in the Stockholm population. An epidemiological study. Acta Ophthalmol (Copenh). 1984 Jun;62(3):378-90. PubMed PMID: 6464687.
- Kanoff JM, Turalba AV, Andreoli MT, Andreoli CM. Characteristics and outcomes of work-related open globe injuries. Am J Ophthalmol. 2010 Aug;150(2):265-269.e2. doi: 10.1016/j.ajo.2010.02.015. Epub 2010 Jun 3. PubMed PMID: 20522411.
- Sweet PH 3rd. Occult intraocular trauma: evaluation of the eye in an austere environment. J Emerg Med. 2013 Mar;44(3):e295-8. doi: 10.1016/j.jemermed.2012.09.028. Epub 2012 Dec 8. PubMed PMID: 23232155.
- Crowell EL, Koduri VA, Supsupin EP, Klinglesmith RE, Chuang AZ, Kim G, Baker LA, Feldman RM, Blieden LS. Accuracy of Computed Tomography Imaging Criteria in the Diagnosis of Adult Open Globe Injuries by Neuroradiology and Ophthalmology. Acad Emerg Med. 2017 Sep;24(9):1072-1079. doi: 10.1111/acem.13249. Epub 2017 Aug 21. PubMed PMID: 28662312.
- Harrahill M. Review of a ruptured globe eye injury: the case for early consult from ophthalmology. J Emerg Nurs. 2005 Aug;31(4):408-10. PubMed PMID: 16126114.
- Ari, A. B. (2006). Eye injuries on the battlefields of Iraq and Afghanistan: Public health implications. Optometry – Journal of the American Optometric Association, 77(7), 329-339. doi:10.1016/j.optm.2006.03.015
