Author: ENS Dylan Hendy, MSIV
Arizona College of Osteopathic Medicine
Author: LT Christopher D. Helman, DO
Naval Medical Center Portsmouth
Originally Published: Modern Resident, April/May 2013
Patient Vignette
Twenty-nine-year-old male was sent to the ED by a community clinic for a syncopal episode. The patient originally visited the clinic for a headache that resulted from a shelf falling on the back of his head while working in his garage two days earlier. The patient denies losing consciousness, amnesia, disorientation or N/V. However, upon further questioning the patient described an unwitnessed episode of “blacking out” while sitting in his car today. He states this episode may have lasted for 30-60 minutes. The clinic subsequently sent the patient to the ED for further workup. In the ED the patient explained that he has a history of chronic headaches and that his headache at present is similar with regards to onset, location and duration. However, to the best of his knowledge, today’s unwitnessed syncopal episode was a first time occurrence. Further ROS were negative. The patient has no other pertinent PMH and is taking no medications. Complete physical exam was unremarkable. A workup for a closed head injury and syncopal episode was performed. Laboratory data was WNL. Non-contrast CT head and CXR were both unremarkable. The following ECG was obtained:
 |
| Image Credit: Modern Resident |
Question
What is the most likely diagnosis?
A) ST elevation myocardial infarction
B) Right bundle branch block
C) Brugada’s Syndrome (BS)
D) Wolff-Parkinson-White Syndrome
Answer
(C) Brugada’s Syndrome (BS). The patient was referred to the emergency department (ED) for an unexplained syncopal episode. In the ED, BS is often diagnosed in patients presenting with unexplained syncope and abnormal ECG findings including ST elevations in V1-2 with an incomplete RBBB pattern.
Brugada’s Syndrome results from a genetic defect in sodium channels and is more common in males and the Asian population. The most worrisome clinical manifestations of BS are ventricular arrhythmias or sudden cardiac death. There is a familial occurrence in up to half of the patients presenting with BS, however, patients who lack a family history should not be assumed low risk.
There are three types of Brugada patterns found on ECGs and these can be differentiated by observing the ST changes in leads V1-V3.
- Classic Type 1 Brugada Pattern: referred to as the “coved type,” with ST elevation >2mm that gradually descends into a negative T wave.
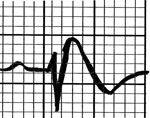 |
| Image Credit: Modern Resident |
- Type 2 and Type 3 Brugada Pattern: referred to as “saddle back,” with ST elevation >2mm and a biphasic T wave creating the “saddle back.” If the terminal portion of the ST segment is >1mm then it is a Type 2 pattern, and if the terminal portion of the ST segment is <1mm then it is Type 3 pattern.
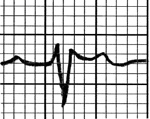 |
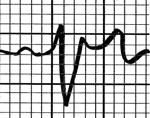 |
| Image Credit: Modern Resident | Image Credit: Modern Resident |
Our patient most likely has a Type 2 Brugada pattern. Refer to the images in your emergency medicine text to assist in further differentiating the three types of Brugada patterns. It is important to note that the Brugada pattern is often transient and episodic.
Patients who have findings concerning for BS require admission and further evaluation with electrophysiology testing. Pharmacologic therapy has been unsuccessful in preventing sudden cardiac death. Insertion of an implantable cardioverter-defibrillator is the current consensus for long-term care.
Reference:
1. Mattu, A. (2012). Brugada Syndrome [Online video]. Retrieved January 15, 2013, from http://www.mededmasters.com/brugada-syndrome.html.
2. Frackelton, M. Chapter 77. Dysrhythmias. In: Marx: Rosen’s Emergency Medicine, 7th ed. Philadelphia, PA: Mosby Elsevier; 2010.
3. Walker RA, Adhikari S. Chapter 22. Cardiac Rhythm Disturbances. In: Tintinalli JE, Stapczynski JS, Cline DM, Ma OJ, Cydulka RK, Meckler GD, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 7th ed. New York: McGraw-Hill; 2011.
4. Wylie, J. V., Pinto, D. S., & Josephson, M. E. (2012, August 29). Brugada Syndrome. In UpToDate. Retrieved January 15, 2013, from UpToDate.
