 |
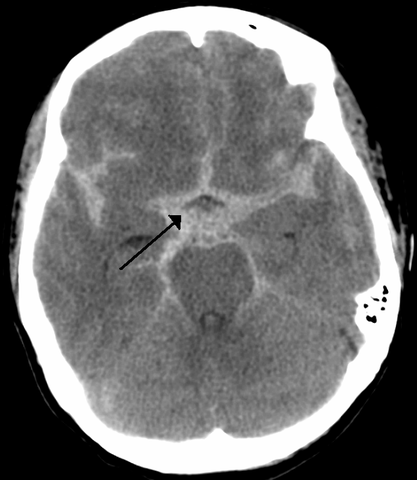
| Photo: Wikimedia Commons |
Originally Published: Common Sense, Jan/Feb 2012
Original Authors: Samantha Wood, MD; Michael Allison, MD; Adam Brenner, MD; Michael Scott, MD; Daniel Boutsikaris, MD; Chris Doty, MD FAAEM; and Michael Bond, MD FAAEM
Headache is a common symptom encountered in the emergency department (ED), representing about 2% of all presenting complaints.(1) Subarachnoid hemorrhage (SAH) is a neurosurgical emergency and is diagnosed in about 1-3% of such ED patients. Guidelines for evaluation and diagnosis of subarachnoid hemorrhage published in 2009 emphasize the need to maintain a high level of suspicion for SAH in patients with an acute severe headache and recommend evaluation with head computed tomography (CT) scan followed by lumbar puncture (LP) if the CT scan is negative.(2)
High risk clinical characteristics for subarachnoid haemorrhage in patients with acute headache: prospective cohort study. Perry JJ, Stiel IG, et al. BMJ 2010; 341:c5204.
Clinical decision rules have been created for a variety of ED complaints. These rules serve to identify patients who are at low risk for certain disease processes and can reduce testing. Investigators from the University of Ottawa, who have previously described clinical decision rules for the ankle, knee, cervical spine and head trauma, set out to find a set of clinical characteristics that can identify
patients with headache who need a workup for SAH.
This multicenter study was performed in Canada. It was a prospective investigation that included all alert (GCS 15) adult patients (>16 years age), who had a chief complaint of headache that was nontraumatic and reached peak intensity within one hour of its onset. Also included was any headache that resulted in syncope. It is important to note those patients who were not included in the study population. Excluded patients were those who presented more than two weeks after headache onset, those with prior SAH, those returning for headache after a complete headache workup with CT and/or LP, those with three headaches of a similar character within the past six months, any patient with papilledema or a focal neurological symptom, or those with history of hydrocephalus or cerebral neoplasm.
The study included 1,999 patients, 130 of whom were diagnosed with SAH. The definition of SAH included any subarachnoid blood on non-contrasted CT of the head, xanthochromia in the CSF, or
RBC > 5x 10^6/L in the final sample of cerebrospinal fluid along with an aneurysm or AV malformation on cerebral angiography. The sample size was calculated a priori to establish a decision rule with 100% sensitivity. Physicians screened patients during their regular work shifts for inclusion in the study. A data form containing 33 clinical findings was completed by the investigating physician and repeated by a second physician if one was available. Patients were followed up with phone calls at one month and six months from their enrollment.
Recursive partitioning was used to find the most predictive variables of SAH. Three clinical decision rules were developed (listed below) and internally validated based upon their data set of nearly 2,000 patients.Each rule contains just four clinical variables:
1. age over 40, neck pain or stiffness, witnessed loss of consciousness, exertional onset
2. arrival by emergency medical services, age over 45, vomiting at least once, diastolic blood pressure >100 mm Hg
3. arrival by emergency medical services, age 45 to 55, neck pain or stiffness, systolic blood pressure >160 mm Hg
Sensitivity of each rule was 100% (CI 97%-100%), and specificities varied from 28.4% to 38.8%. Presence of one or more findings should prompt workup for SAH. If none of these variables were present, then physicians could reliably rule out SAH with near certainty. These rules would lower the current utilization of CT and LP in the study population by 10-20% in absolute terms.
The main limitation of this study was that up to 1/3 of eligible patients may not have been enrolled. These patients had very similar characteristics to the study population in terms of age, gender and arrival by ambulance. Of the non-studied population of potentially eligible patients, 2.7% were diagnosed with SAH compared with 6.5% of the study population, suggesting perhaps that this was a lower acuity population that was missed.
This study may prove to be groundbreaking, as it may lead to more selective workup for headache without missing SAH, thus reducing the need for diagnostic tests and decreasing ED length of stay for patients with headaches. Though promising, these results need to be prospectively validated in more than one setting. The Ottawa group is currently conducting such a study using each of the three clinical decision rules, with the hope of identifying one rule with 100% sensitivity. Clinicians should recognize patients with the above-mentioned features and carefully consider them for SAH workup; however, these rules are not yet ready for clinical application.
Trigger factors and their attributable risk for rupture of intracranial aneurysms: a case-crossover study. Vlak M, Gabriel J, et al. Stroke 2011; 42: 1878-1882.
Although aneurysm rupture can occur at any time, it may also be preceded by various stressors that are thought to cause the rupture. This study investigated patients with SAH and their exposure to trigger stressors shortly before symptom onset in comparison to their usual exposure to the same stressors.
Adult patients (greater than 18 years of age) who were admitted to a stroke center in the Netherlands with aneurysmal SAH were asked to complete a questionnaire regarding the circumstances surrounding the onset of their headache. They were asked about their exposure to several stressors within a defined “hazard period” leading up to their symptoms. Trigger stressors and their respective hazard periods included valsalva, heavy lifting, strong emotions,sexual activity, temperature change, vigorous physical exercise, use of tobacco or caffeine (hazard period of one hour); use of cocaine, marijuana, or sildenafil (hazard period of four hours); and fever, flu-like symptoms, and use of alcohol (hazard period of 24 hours). Patients were also asked to describe their “usual exposure” to these stressors. Patients who gave inconsistent answers when similar questions were phrased differently were excluded from the analysis.
Two hundred and fifty patients were included in the analysis. Relative risk was calculated for each stressor. Reported stressors found to be statistically associated with triggering of an aneurismal rupture included drinking coffee or cola, nose-blowing, straining for defecation, startling, anger, sexual intercourse and vigorous to extreme physical activity.
The main flaw of this study is the potential for recall bias. Another significant flaw is the failure to collect data on the most seriously ill patients or those who died (171 patients were excluded from the
study due to death or severe disability). However, the less severely ill patient population that participated in the study represents the group in whom there is the greatest concern about missing the
diagnosis of SAH in the ED. A final consideration is that it is not known what the specificity or sensitivity of these symptoms are for SAH as compared to other types of headaches.
The authors speculate that the association of the trigger stressors with SAH reflects the transient rise in blood pressure that accompanies most of the trigger exposures and suggest measures to reduce these exposures in patients with known SAH (e.g., eliminate caffeine, reduce constipation with stool softeners). For the emergency provider, this study is perhaps more useful as yet another reminder of the importance of history in making the diagnosis of SAH. As a small component of a thorough history, we should consider a patient’s exposure to these stressors in the time leading up to the onset of their headache.
The next two articles investigate the sensitivity of modern CT in the diagnosis of SAH.
Given the substantial morbidity and mortality associated with SAH, the timely application of diagnostic modalities with sensitivity approaching 100% is paramount. Traditionally, initial diagnostic evaluation for SAH begins with non-contrast head CT, followed by LP if the head CT yields negative results. However, there are many drawbacks associated with the LP, including patient pain, discomfort and anxiety, the potential for complications, as well as time constraints inherent to the ED. The following two studies evaluate the sensitivity of modern head CT in the evaluation of SAH and consider the possibility that an LP may not be necessary if a CT performed within a certain period of time from symptom onset can be shown to have adequate sensitivity for excluding SAH.
Sensitivity of computed tomography performed within six hours of onset of headache for diagnosis of subarachnoid haemorrhage: prospective cohort study. Perry JJ, Stiel IG, et al. BMJ 2011; 343:d4277.
This prospective multicenter cohort study enrolled 3,132 alert, neurologically intact patients presenting with high risk headache. “Alert” was defined by a Glasgow coma score (GCS) of 15; “high risk” was defined as an atraumatic headache reaching maximal intensity within one hour or an atraumatic headache associated with syncope. The primary outcome was SAH, defined by the detection of subarachnoid blood on CT, xanthochromia identified in CSF, or any red blood cells detected in the final tube of CSF in conjunction with aneurysm identified on cerebral angiography.
Overall, of the 3,132 patient cohort, 240 (7.7%) were found to have SAH. A subset of 953 patients had head CT performed within six hours of headache onset; of these, 121 patients were diagnosed with SAH, and all cases were identified on head CT with 100% sensitivity (95% CI, 97-100%). At greater than six hours (n=2,179), the sensitivity was 85.7% (95% CI, 78.3-90.9%); the overall sensitivity of head CT among this cohort was 92.9% (95% CI, 89-95.5%). All studies were performed with third generation modern multi-slice scanners and interpreted by experienced local neuroradiologists or general radiologists who had access to pertinent clinical information but were blinded to patient participation in the study. Local laboratory technicians unaware of the study interpreted CSF for xanthochromia by visual inspection. Patients who did not have a definitive cause of their headache diagnosed in the ED were followed over six months; of the 1,931 patients in this category, 31 were lost to follow up, and none of the remaining patients were identified as having an SAH.
The study examines an extremely relevant clinical scenario in emergency medicine and includes a notably high risk headache patient cohort, as evidenced by the overall percentage (7.7%) of
patients definitively diagnosed with SAH. There are, however, several limitations of this study. A CT in one patient presenting approximately 4.5 hours after headache onset was initially misinterpreted as
normal, though the scan was retrospectively re-read as positive for SAH after an aneurysm was identified on cerebral angiography. In addition, not all patients with a normal head CT underwent LP, and therefore, did not receive the gold standard diagnostic test utilized in the study. Further, 13 patients who had a head CT within six hours of headache onset were lost to follow up. Although no cohort subjects were admitted to any regional neurosurgical referral centers, the single misinterpreted CT scan, lack of LP in all patients, and subjects lost to follow up suggest that the sensitivity of this study is more accurately described as approaching 100%, rather than being definitively labeled as 100%. Defining SAH by xanthochromia with visual inspection is also controversial (though it still remains the method used at most centers), and may be inherently biased and operator dependent. Finally, the requirement of a modern generation CT scanner with interpretation by a qualified radiologist limits the applicability of this study to EDs lacking access to such modern scanners and specialists.
Overall, the study demonstrates that the modern generation of CT scanners are extremely sensitive (approaching 100%) for detection of SAH if obtained within six hours of headache onset and when interpreted by qualified radiologists. Further studies with similar results could help remove the requirement for LP in some patients with suspected SAH.
Determining the sensitivity of computed tomography scanning in early detection of subarachnoid hemorrhage. Cortnum S, et al. Neurosurgery 2010; 66: 900-903.
This retrospective chart review study conducted at a single neurosurgical unit examined patients admitted with suspected SAH or verified SAH within a five year enrollment period. Charts were reviewed to determine clinical history, examination findings, time from onset of symptoms to workup, and CT and LP results. All CTs were performed using a modern 64 slice multidetector scanner. SAH was defined by either positive head CT or LP showing xanthochromia by spectrophotometry. Eight patients were excluded because there was no clinical suspicion for SAH and an LP was not performed. Three additional patients were excluded because CT scan revealed an alternative diagnoses.
Overall, 499 patients were included in the analysis, of whom 296 patients were diagnosed with SAH (59%). Most (295) of these patients were diagnosed by CT. In one patient presenting six days after onset of symptoms, the diagnosis was made based upon LP results. CT was found to have a sensitivity of 100% for patients presenting within the first five days of symptom onset. Overall, CT sensitivity was found to be 99.7% (95% CI, 98.1-99.9%).
There are several limitations of this study. First, spectrum bias limits the applicability to ED patients; the study cohort consists of patients accepted to a neurosurgical unit, which represents a different population from undifferentiated headache patients in the ED. Moreover, there is no description of the presenting neurological status of these patients; therefore, it is possible that the study included patients with existing neurological deficits reflecting larger hemorrhages more likely to be visualized on CT. The high rate of SAH (59%) among the patient cohort also reflects an element of spectrum bias. In addition, a positive LP was defined by CSF xanthochromia by spectrophotometry; however, in the United States, most centers utilize visual inspection to determine the presence of xanthochromia, also limiting the applicability to the U.S. patient population. Another limitation is the retrospective nature of a chart review that inherently suffers from both selection bias and referral bias.
Despite these limitations, the authors state that it seems safe to omit lumbar puncture in patients with a negative head CT within three days from symptom onset based on their findings of very high sensitivity of CT in their patient population. Emergency providers must be aware of this data from the neurosurgical literature but must use extreme caution in applying it to the undifferentiated ED patient.
It is important to note again that the Perry study (reviewed above), a prospective investigation, found an unacceptably low sensitivity of head CT for SAH of 85.7% when performed more than six hours after headache onset in patients presenting to the ED.
Evaluating the sensitivity of visual xanthochromia in patients with subarachnoid hemorrhage. Aurora S, Swadron S, et al. JEM 2010; 39: 13-16.
Past studies have found xanthochromia on lumbar puncture to have a sensitivity of 100% for subarachnoid hemorrhage, supporting the critical role of this study in the diagnostic algorithms and clinical guidelines. However, these studies used spectrophotometry to evaluate for the presence of xanthochromia, whereas the vast majority of hospitals (75% as of 2002) use visual inspection of CSF supernatant to determine the presence or absence of xanthochromia.(3) The authors of this article investigated the sensitivity of xanthochromia as determined by visual inspection of CSF.
This was a retrospective chart-review. The initial population pool of 1,323 patients was generated by identifying all patients evaluated in the ED over a 12 year period who were discharged with a diagnosis of SAH. One hundred and two (102) patients had a procedural charge for lumbar puncture or spinal tap. After excluding those patients for whom an official lab report of CSF color was not available, a confirmatory imaging study was not available, and those where the lumbar puncture was performed less than hours or more than two weeks from headache onset; the authors were left with 19 patients with imaging-confirmed SAH who had CSF results available. Nine (47%) of these patients had a positive finding of xanthochromia on visual inspection, while 11 (53%) were found to have clear CSF on visual inspection. The resulting sensitivity of visual inspection of xanthochromia for SAH was 47.3% and is at significant odds with prior studies showing the sensitivity of spectrophotometry determined xanthochromia to be 100%. This suggests that, in the majority of hospitals where spectrophotometry is not used, the absence of xanthochromia cannot be relied upon to exclude SAH.
There are a number of limitations to this study, the most prominent being the small number of patients who were included. However, for a variety of reasons including the sensitivity of CT (which is generally performed as an initial test in the workup of SAH), the pool of patients who both have a positive imaging study and undergo LP is quite small. The authors were also limited by difficulty accessing records and by failure of the laboratory to report CSF color in several cases. They also point out that they were not able to investigate the number of patients discharged with negative CSF results who subsequently were found to have SAH.
Despite these limitations, the number of patients with negative CSF for xanthochromia by visual diagnosis that were found by CT to have a SAH does strongly suggest that this test cannot be relied
upon to exclude SAH. The authors suggest, however, that making spectrophotometry universally available would probably not be costeffective, as its specificity of approximately 75% found in past studies would result in many unnecessary evaluations for SAH, including such costly and/or invasive studies as cerebral angiograms or MRA.
In conclusion, this study suggests that the absence of xanthochromia, when determined by visual inspection, is not sufficient to rule out SAH in headache patients. The emergency provider should be aware of what method for evaluation of CSF is used in his or her hospital and be attentive to the limitations of this result. One also needs to remember that it can take up to six hours for xanthochromia to develop, so an LP done <6 hours from symptom onset may be negative despite the fact that there is an SAH hemorrhage.
Conclusions:
Headache is a common complaint seen in the ED, and SAH is one of the most feared causes of this symptom. Determining who is at risk for SAH, what diagnostic tests are necessary, and how to interpret the results of these tests can be challenging for the emergency physician. Some key points from the above studies are summarized below.
Take Home Points:
• Clinical decisions rules for SAH are not ready for clinical use, but may prove to be an effective method of limiting diagnostic testing while maintaining good sensitivity.
• The current literature shows that the tide may be changing on whether LP should be required in all patients with a negative head CT done on a modern generation multidetector CT scanner within six hours of headache onset.
• Visual inspection of xanthochromia is inherently insensitive, and its absence should not reassure the emergency provider that a SAH is not present.
References:
1. Edlow JA, Panagos PD, Godwin SA, Thomas TL, Decker WW. Clinical policy: critical issues in the evaluation and management of adult patients presenting to the emergency department with acute headache. Ann Emerg Med. Oct 2008; 52(4): 407-436.
2. B ederson JB, Connolly ES, Jr., Batjer HH, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a statement for healthcare professionals from a special writing group of the Stroke Council, American Heart Association. Stroke. Mar 2009; 40(3): 994-1025.
3. Edlow JA, Bruner KS, Horowitz GL. Xanthochromia. Arch Pathol Lab Med. Apr 2002; 126(4): 413-415.
